BREAST CANCER
Breast cancer concerns all women. Each year in our country, there are approximately 4,500 new cases, and it is estimated that 1 in 8 women worldwide will experience breast cancer at some stage in their lives.Medicine has made great progress in relation to its treatment, but the key lies in prevention and early diagnosis.
THE MOST FREQUENT CANCER
Breast cancer is the most common cancer in women in the Western world.It occurs when some breast cells lose control of their multiplication process and divide with no control. These cells have the potential to break - filter some physiological anatomical barriers of the breast and disperse in the rest of the body.
EARLY DIAGNOSIS
Every woman, from the age of 20, should go through a breast self-examination at least once a month, and should visit her doctor for a clinical breast examination every 3 years.After the age of 40, a clinical examination by a doctor should occur annually, and a mammography should be done every year. An annual mammography check should begin even earlier, after the prescription of a specialist, for women with a hereditary history of breast cancer.
SELF-EXAMINATION
Breast self-examination is the first and basic method of preventive breast checking and can be done very simply at home by the woman herself.All women, after the age of 20, need to properly learn how to self-examine their breasts.
The secret for every modern woman is to diagnose the disease at an early stage. Early diagnosis of breast cancer is the golden rule. The sooner we find it, the better the following course will be.
SYMPTOMS
Many breast tumors do not cause any symptoms. For example, they can be diagnosed with a mammography on a woman that has not experienced any symptoms.It is very important for every woman to be familiar with her breasts so that she can detect any changes.
Modern laboratory and paraclinical examinations help to discover tumors of very small dimensions, which can be treated extremely well.

BREAST & DISEASES
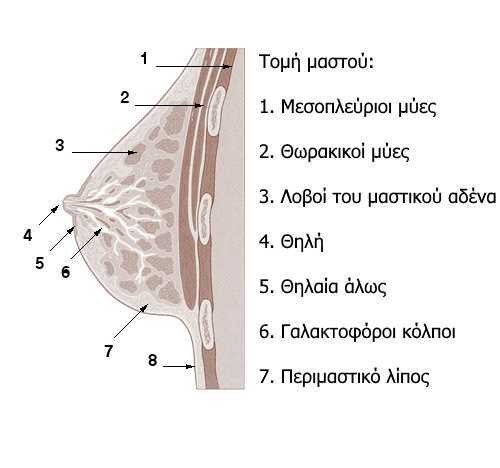
THE EXTERIOR BREAST
The external morphology of the breast includes the nipple, the areola and the areola nodules.
THE NIPPLE
The nipple is an imprint of the skin of the breast that is just below and in the outer part of the middle of the breast. At the top there are 15-20 nozzles where milk pores end up. The height of the nipple is about 1-1.5 cm and it increases during breastfeeding. The brownish color of the nipple is related to the abundant presence of the substance melanin. The areola is the subcircular and slightly elevated area around the nipple with a diameter of 1.5-6 cm. On the surface of the areola, there are small elevated points, the areola nodules which are supported by the areola glands. The areola glands are mainly scent glands, but also sebaceous and rudimentary lactic glands.
THE INTERNAL OF THE BREAST
Internally, the breast consists of the mammary or mass gland and the peritoneal fat. Peritoneal fat is a continuation of the subcutaneous fat, but it is more abundant in the anterior region of the breast, between the skin and the mammary gland.
THE MAMAMRY GLAND
The mammary gland in a non-pregnant woman is located behind the areola and just beyond its limits. The mammary gland consists of the lobes, where the milk is produced, and of milk pores that transfer the milk to the milk storage areas. Milk glands are aneurysms of pores that act as storage area for the milk, which they release after the infant applies pressure to the nipple.
The layer consists mainly of dense fibrous and connective tissue mixed with fat tissue.
Under normal circumstances, the glandular tissue is subject to changes associated with the hormonal changes of the menstrual cycle.
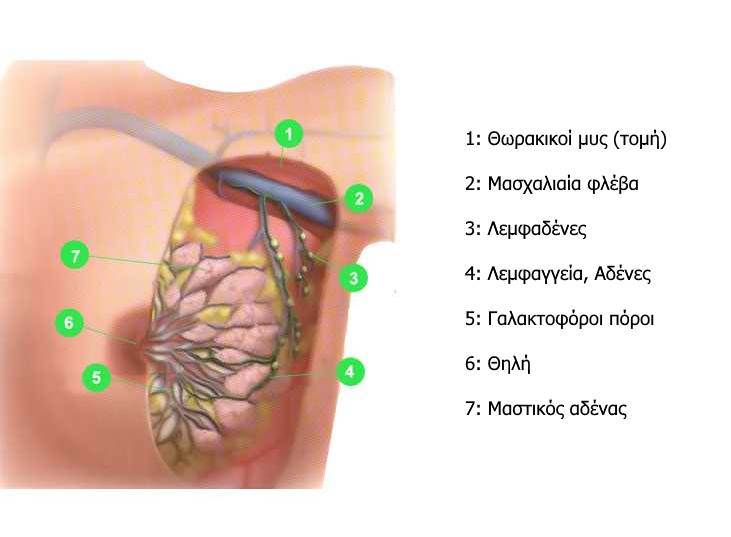
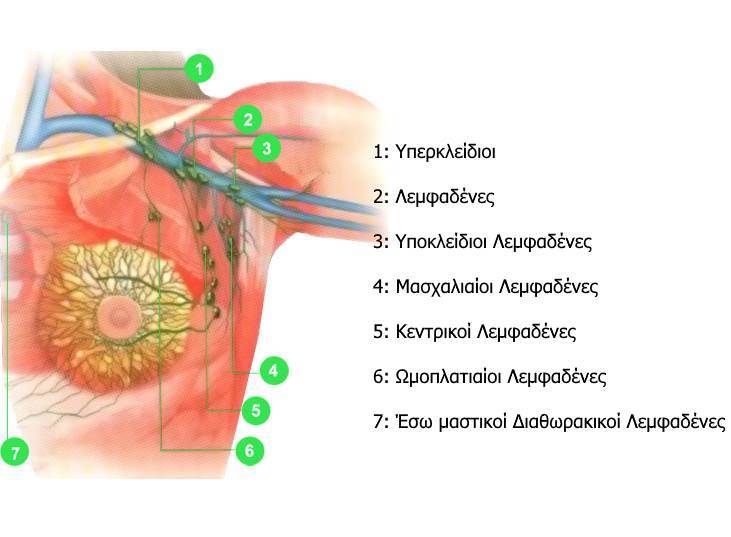
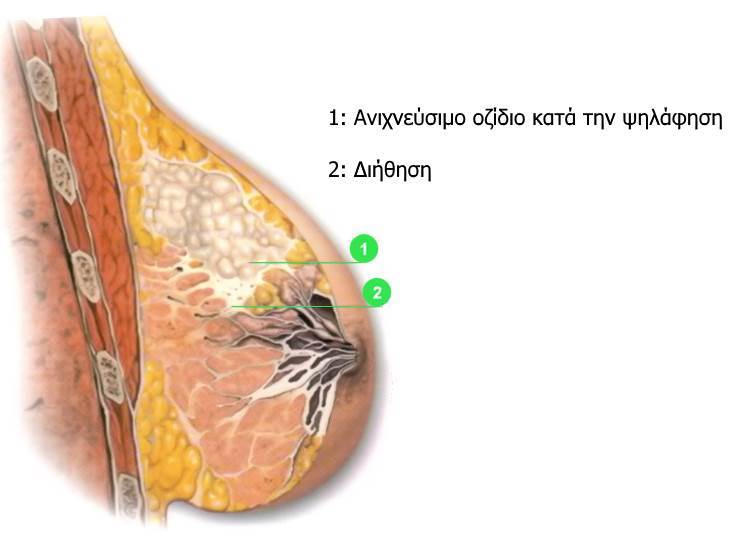

In most cases, invasive lesions appear in the epithelium of the lobes and pores and include: hyperplasia, atypical hyperplasia, in situ carcinoma and invasive carcinoma.
In 85% - 90% of the cases of invasive carcinomas, they are porous carcinomas.
From a therapeutical point of view, breast cancer can be classified into: non-invasive carcinoma - locally-localized carcinoma with the possibility of exclusion by excision or not and recurrent or metastatic carcinoma.
When a palpable mass is found in the breast, the steps to be followed should be adapted to the age of the patient, the results of the examination and the risk factors.
The initial assessment in women under 30 years of age should include ultrasound examination of the breasts or suction biopsy techniques • in the case of a suspicious mass, a mammography is recommended before conducting a biopsy or a needle aspiration.
In women over 30 years of age, a mammography is recommended to evaluate both breasts - ultrasound examination may help distinguish between solid and cystic masses.
Thin-needle biopsy is also an important procedure in the initial assessment of palpable mass in the breast.
Breast biopsy without surgery
Our clinic has been implementing the innovative method of stereotactic biopsy with a type of device that uses an incision in the breast.
With this method we can take a small piece of breast and analyze it under the microscope in order to obtain a bloodless diagnosis for some breast disorders.
This diagnostic method is the spearhead of modern mammology at international level and our team has the honor to be the first in the private sector to apply it.
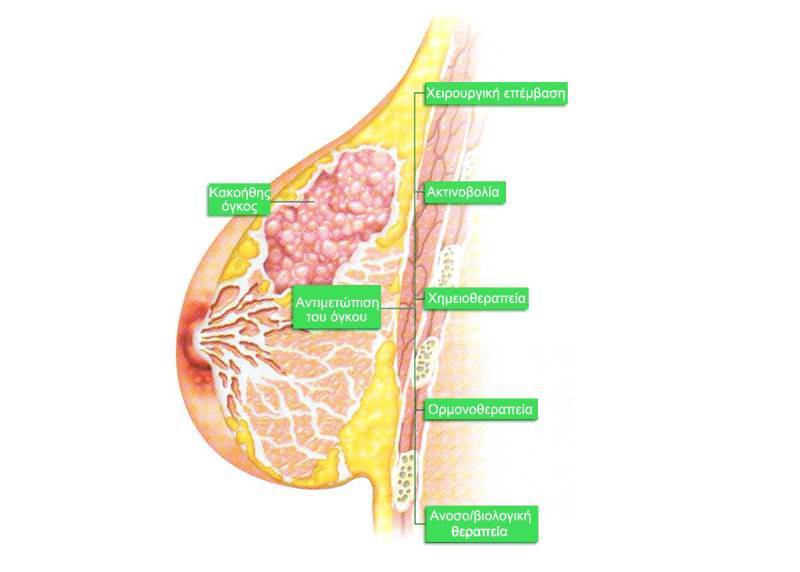
General aspects
As far as concerns breast cancer, the choice of treatment depends on a few factors: the clinical and histopathological characteristics of the primary tumor and of the armpit lymph gland, the presence of hormone receptors, the level of expression of the HER2/neu gene, the existence of metastases, the associated commorbidity, the age of the patient and the presence or absence of menopause.
The treatment includes topical treatment of the disease by surgery, radiotherapy or both.
In case of a metastasis, the indications include chemotherapy, hormone therapy, biological therapy or a combination of all these strategies.
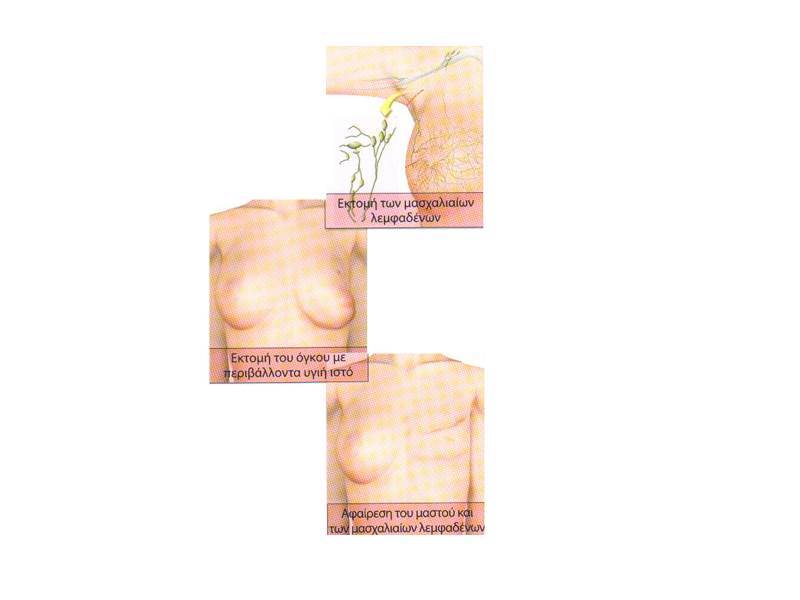
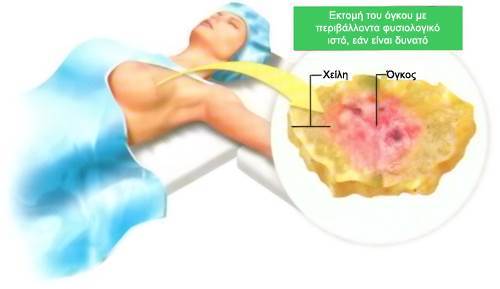
Although the modified radical mastectomy was the usual treatment for breast cancer for decades and is still indicated in some cases, conservative treatment has become the selected method for many patients.
This consists of the resection of the primary tumor with the neighboring mammary tissue, often followed by a radiotherapy.
This kind of surgery is also widely known as tumor excretion or partial or sectional mastectomy.
SENTINEL LYMPH NODE
SENTINEL LYMPH NODE
Each year in our country approximately 4,000 women are affected by Breast Cancer, which is the most common malignant tumor concerning the female population. The establishment of preventative controls with breast clinical examination and mammography, will give an early diagnosis of the tumor at an "early" stage, with an excellent prognosis for the patient, also allowing breast preservation.
For the application of the cure, in addition to removing the tumor, the removal of the armpit gland is necessary in order to determine the possible presence of cancer in the lymph nodes. This operation - lymphatic cleansing – most of the time is used not as a prognostic but as a therapeutic process, but it causes to some extent undesirable effects such as numbness and limb weakness, shoulder stiffness, and sometimes lymphoedema.
The possibility of filtration of the armpit lymph nodes increases proportionally to the size of the tumor. However, the implementation of preventive control programs increasingly leads to the diagnosis of breast cancers of small size and therefore with less chances to have filtered lymph nodes. Thus, a large proportion of patients are subjected to lymph node removal only to confirm that no metastasis has occurred.
In recent years, attempts have been made to find methods to determine the presence or absence of metastases in the armpit lymph nodes without their surgical exclusion, to avoid the complications of a possibly unnecessary intervention. The application of the sentinel lymph node technique solves a large number of these cases.
The sentinel lymph node is considered the first lymph node - metastasis station in which the area of the cancer drains and the first among the other armpit lymph nodes that will receive a cancer cell metastasis. If it results 'negative', it determines with a probability that reaches the 96-97% that the other lymph nodes are also clear of cancer cells and they do not need to be removed.

According to international scientific data, we use a combination of three methods:
1. Imaging of the lymph node with radioisotope: this is done one day before the surgery, in the Nuclear Medicine section. We inject into the breast a small amount of radioisotope. This medicine is transported by the lymph nodes and connects to the sentinel lymph node. With the help of a scintigraphy, we identify this lymph node and mark its position. This radioactive material is absolutely safe for you and your family members.
2. Pigment labeling: in the operating room, after the general anesthesia, we add a small amount of a specific blue pigment to the breast. This blue liquid is transported with the lymph nodes and ends up in the sentinel lymph node, which gets colored in blue. This makes it easier to locate it during its surgical removal. This pigment is absorbed by the body and is removed with the urine. A small blue hue may remain in your skin for a few weeks.
3. Tracking with a detection device: with a special sensitive detector, we locate the sentinel lymph node that has trapped the radioisotope medicine. So, we are sure that we are doing a biopsy on the right lymph node.
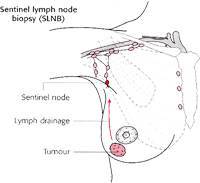
The lymph nodes are some small organs that filter the lymph, the fluid that carries the metabolic products of all organs. Their most important task, however, is that they participate in the body's defense when it faces dangers such as the infection or the spreading of a tumor.
When a tumor exists in the breast, the first armpit lymph node that receives the lymph of the area can become a tumor cell receptor. This lymph node, as it is the first one, is called "sentinel lymph node".
During the biopsy, we remove this lymph node and examine it pathologically and anatomically to see if it contains cancer cells or not.
Why is it important to know if there are cancer cells in the sentinel lymph node?
The presence of cancer cells in the lymph node is an indication that this tumor has an increased risk of being transferred also to other lymph nodes. It is important to know this for us to better plan your treatment.
How fast are biopsy results obtained?
Once removed, the lymph node is examined by a doctor-pathologist with a microscope. A rapid histological and cytological evaluation is performed, which at the 80% of the cases reveals the presence of tumor cells.
In these cases, we proceed immediately to a full surgical cleansing of the armpit. Then, a complete histological evaluation is required, which takes 10-14 days.
At the small rate that the rapid biopsy does not give results, we may need to modify the treatment or undertake a surgical armpit cleansing later.
Will the biopsy result determine whether I will do a full or partial mastectomy?
No. The result of the biopsy determines if the surgical cleansing of the armpit will occur or not, but not the breast operation.
Is the radioisotope harmful?
The dose of radiation you receive is minimal, equal to a mammography and much smaller than an axial tomography.

What are the advantages of the lymph node biopsy?
It is a very reliable method for the determination of the stage of the disease. It is a much smaller procedure than the surgical cleansing of the armpit lymph nodes, so we have a smaller scar, less pain, better and faster healing and we avoid unpleasant complications.
What are the disadvantages of the biopsy of the sentinel lymph node?
In less than 5% of the cases, the method may result unsafe. This means that in a minimal number of cases, although the lymph node biopsy may result negative, there may be some small hosts in other lymph nodes.
The blue pigment can remain for a few weeks on the breast skin, but ultimately it is absorbed by itself.
Cases of allergy (less than 1%) in the blue dye have been reported, but these are treated immediately and effectively during surgery.

How much safe is the process?
The team of Grigoris Xepapadakis follows the protocols of the Royal College of Surgeons of England and is under his supervision for the proper observance and processing of the procedure. In addition, shortly our Clinic will be the control and training center of the College of Surgeons of England in Greece.
What if the lymph node is affected by the tumor?
We will need to undergo full surgical cleansing or radiotherapy at the armpit.
What will happen if I reject to undergo a sentinel lymph node biopsy?
The decision to do the biopsy or not is entirely yours. If you decide not to go ahead with the biopsy, let us know and we will suggest alternative solutions.
